
Share
![]()
Written by Occupational Therapist, Lucinda Blundell
Wheelchair seating plays an important role in comfort, function and postural support—but it’s only one part of the picture.
For many people with disability, overnight positioning can influence how the body presents the next day. A person may spend 8–12 hours in bed, and without adequate support, the lying posture can reinforce asymmetry, rotation or discomfort.
That’s why 24-hour postural management considers the full day and night. It looks at how a person is supported while lying, sitting, standing, transferring, toileting and resting, so equipment and support routines work together.
For Occupational Therapists, support workers and family members, this approach can help improve comfort, protect body shape and support more consistent functional outcomes.
Why overnight positioning matters
A carefully prescribed seating set-up can only do so much if a person spends long periods overnight in an unsupported position. When a person sleeps in a rotated, asymmetrical or poorly supported posture, those positions may carry over into the next day and influence daily function, including transfers, self-care, tolerance for school or work, communication, wheelchair comfort, and morning routines.
Posture is not limited to sitting; it’s shaped by how the body is aligned and supported across lying, sitting and standing. It’s also influenced by the surfaces a person uses throughout the day, including beds, wheelchairs, lift chairs, shower commodes and standing supports.
Many people shift, stretch and readjust without thinking. They may roll in bed, change how they sit, or stand when a position becomes uncomfortable. For people with disability, altered tone, reduced joint range, reduced strength or motor control limitations can make these small protective movements much harder.
Over time, limited repositioning can increase the risk of asymmetry, contracture and secondary complications. It may also affect breathing, swallowing, comfort and overall function.
This is where assistive technology and clear support routines can play an important role. When they’re prescribed and used consistently, they can help support alignment, comfort and function across the full 24 hours.
What is 24-hour postural management?
24-hour postural management involves assessing a person’s postural needs across the full 24-hour period. It considers how they are supported in lying, sitting, standing and, where relevant, walking.
The goal is to create practical strategies that support the person across different environments. This may include prescribed equipment, positioning routines, support worker training and review plans.
Depending on the person’s needs and goals, 24-hour postural management may help:
- Support daily function and participation
- Assist motor development and reduce the impact of atypical movement patterns
- Support comfort, rest and relaxation
- Help prevent or minimise secondary complications, such as contracture, deformity or hip displacement
- Manage pressure distribution and support skin integrity
- Support breathing, swallowing and digestion
- Improve consistency between seating, sleeping, toileting and transfer routines
For many wheelchair users, prolonged time in sitting and lying positions means postural support needs to remain consistent across the full day. Seating should not be viewed in isolation from what happens overnight.
What are sleep systems?
A sleep system, also called a night-time positioning system, is a set of prescribed supports used in bed. It helps a person maintain a stable, comfortable and more symmetrical lying position during sleep or rest.
A sleep system may include a mattress or overlay, wedges, bolsters, cushions and other positioning supports. These components are selected and arranged to suit the person’s posture, comfort, pressure care needs and support environment.
Sleep systems are often considered for people who can’t reposition independently during the night. They may help support alignment, comfort, skin protection and body-shape management over longer periods of rest.
What does the research say about sleep systems?
The evidence base for sleep systems is still developing. Large randomised controlled trials are limited, and much of the available research is based on case studies, pilot studies or specific clinical populations.
Current research is weighted toward people with cerebral palsy and neurodisability. This means the findings are useful, but they shouldn’t be treated as a one-size-fits-all answer.
Research and clinical reports have identified potential benefits across posture, comfort, pain, range of motion, hip positioning, sleep quality, pressure care and ease of support routines. However, outcomes vary between individuals. For this reason, sleep systems should be prescribed based on the person’s presentation, goals, tolerance and support environment.
Early review is also important after introduction, particularly for comfort, skin response and respiratory tolerance.
Potential benefits of sleep systems
Research and clinical practice suggest that sleep systems may support several areas of function and care, as highlighted below.
Body alignment and range of motion
Sleep systems may help a person maintain a more symmetrical lying position overnight. This can support lower-limb range of motion and may assist with contracture management as part of a broader 24-hour postural management plan.
Comfort and pain management
Several studies associate sleep system use with reduced pain or improved comfort. Improved positioning may reduce pressure on sensitive areas and help the body rest in a more supported position.
Tone and spasm management
Some reports suggest that night-time positioning may help reduce tone or spasms for some users. This may support a more relaxed overnight positioning and better tolerance during the day.
Hip and joint positioning
Sleep systems may form part of an orthopaedic risk management plan, particularly where hip positioning, hip migration or joint range are key clinical considerations.
Pressure redistribution and skin integrity
By improving posture and supporting load distribution, sleep systems may help reduce pressure over bony prominences. Skin response should still be monitored closely, especially when a new system is introduced.
Daytime positioning and function
Better overnight positioning may support better carryover into wheelchair seating, shower commode positioning and transfers. This may help simplify equipment needs and improve functional consistency over time.
Support routines and morning care
Sleep systems may make morning routines easier for support workers and family members. This may include positioning for dressing, washing, toileting and sling application.
Sleep quality and daytime alertness
Findings around sleep quality are mixed. Some research reports similar or improved sleep, while other research does not show a significant difference in sleep disturbance. Sleep quality should be considered alongside posture, comfort, function and support goals.
What does this mean functionally?
The potential outcomes above matter because posture affects participation.
When pain, tone or spasm reduces, a person may have better tolerance for daily activities. This may support sitting tolerance, hand use, communication, play, learning, work, transfers and personal care. For some people, reduced tone or improved comfort may also broaden functional goal setting.
Overnight positioning may also influence the support required during the day. If a person is easier to position on a commode, has improved comfort, or needs less time for transfers, daily routines may become more efficient for support workers and family members.
In some cases, improved carryover from night-time positioning may also support equipment planning. More complex postural presentations often require more customised seating solutions. Supporting posture overnight may help reduce the risk of daytime seating goals being undermined by unsupported lying positions.
Overnight positioning can also be clinically useful because the body has fewer functional demands during sleep. Longer periods of supported contact may provide an opportunity to use gravity therapeutically and support more symmetrical alignment.
Further research is needed across a broader range of client groups. However, current findings support the value of considering sleep positioning as part of a complete 24-hour postural management approach.
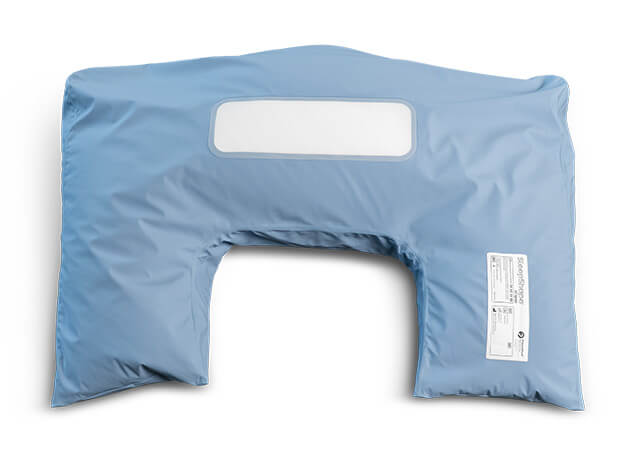
Product spotlight: SleepShape by SPEX Cushions


Active Mobility offers the SleepShape by SPEX range of positioning cushions to support 24-hour postural management needs.
SleepShape positioning cushions are designed to support postural alignment in the lying position. They’re available with microbead or microfibre filling and a choice of comfort or wipeable covers, and come in a range of cushion shapes, sizes, and covers. These options allow components to be selected based on the person’s clinical presentation, support environment and comfort needs.
The range also includes small targeted supports through to larger full-body profiles. The aim is to support alignment, comfort and pressure redistribution for people who are unable to reposition independently.
Benefit #1: Versatile range of shapes, from simple to more complex contours

Benefit #2: Choice of microbead or microfibre fillings

Benefit #3: Adjustable microfibre volume to suit individual postural needs

Benefit #4: Comfort fabric and wipeable cover options for easy cleaning and infection control

Benefit #5: Durable design for long-term clinical use

Benefit #6: Clear cushion identification to support easier set-up and management

Benefit #7: Hygienic covers are also available
Clinical considerations when prescribing sleep systems
Sleep systems should be prescribed as part of a clear clinical plan. Key considerations include:
- Clarify the goal: Confirm whether the main aim is body-shape protection, range of motion maintenance, tone management, pain reduction, skin protection, respiratory support, easier handling, or carryover into daytime positioning
- Set a baseline: Document posture, range of motion, pain behaviours, sleep tolerance and current sleeping patterns, skin integrity and support worker or family member feedback before the system is introduced
- Agree on review measures: Set clear timeframes and outcome measures so changes can be monitored
- Introduce gradually where needed: Consider a staged build-up if prolonged positioning is new for the person
- Monitor comfort and skin response: Check pressure areas, bony prominences and overall tolerance during the introduction phase
- Consider respiratory needs: Where respiratory compromise is present, confirm the proposed position does not negatively affect ventilatory function. A multidisciplinary approach may be required to monitor ideal postural positions to optimise respiration
- Integrate the full 24-hour plan: Align sleep positioning with wheelchair seating, shower commode positioning, transfers and manual handling routines
Better sleep positioning starts with the full 24-hour picture
Wheelchair seating is only one part of a person’s total postural exposure. For many people, 8–12 hours of overnight positioning can either reinforce asymmetry or support alignment goals.
If persistent postural asymmetry is affecting comfort, function or seating outcomes, lying posture should be reviewed as part of the broader 24-hour postural management plan. Assessing and supporting overnight posture can make a meaningful difference to comfort, body-shape protection, care routines and daytime function.
To discuss a client’s positioning needs, trial SleepShape by SPEX positioning cushions, or explore how overnight positioning can support an existing seating plan, contact Active Mobility today.
References
- Owens, K., & Daly, G. (2017). A study into the effectiveness of 24 hour postural care in the management of contractures in care homes [Report]. Middlesbrough Social Care.
- Gericke, T. (2006). Postural management for children with cerebral palsy: Consensus statement. Developmental Medicine & Child Neurology, 48(4), 244.
- Dawson, N. C., Padoa, K. A., Bucks, R. S., Allen, P., Evans, H., McCaughey, E., & Hill, C. (2013). Ventilatory function in children with severe motor disorders using night-time postural equipment. Developmental Medicine & Child Neurology, 55, 751–757.
- Innocente, R. (2014). Night time positioning equipment: A review of practices. New Zealand Journal of Occupational Therapy, 61(1), 13–19.
- Aburto, N., & Brown, S. (2014). Pilot research study into the effects of sleep systems on quality of sleep, pain and joint range [Report]. Hounslow Wheelchair Service.
- Humphreys, G., King, T., Jex, J., Rogers, M., Blake, S., Thompson-Coon, J., & Morris, C. (2019). Sleep positioning systems for children and adults with a neurodisability: A systematic review. British Journal of Occupational Therapy, 82(1), 5–14.
- Hill, C. M., Parker, R. C., Allen, P., Paul, A., & Padoa, K. A. (2009). Sleep quality and respiratory function in children with severe cerebral palsy using night-time postural equipment: A pilot study. Acta Pædiatrica, 98, 1809–1814.
- Hankinson, J., & Morton, R. E. (2002). Use of a lying hip abduction system in children with bilateral cerebral palsy: A pilot study. Developmental Medicine & Child Neurology, 44(3), 177–180.
- Pountney, T. E., Mandy, A., Green, E., & Gard, P. R. (2009). Hip subluxation and dislocation in cerebral palsy: A prospective study on the effectiveness of postural management programmes. Physiotherapy Research International, 14(2), 116–127.
- Wynn, N., & Wickham, J. (2009). Night-time positioning for children with postural needs: What is the evidence to inform best practice? British Journal of Occupational Therapy, 72(12), 543–550.
- Neylon, S. (2013). Developing and testing the adaptability and utilisation of care workers as part of an interdisciplinary workforce model of practice [Abstract]. Health Workforce Australia; Brightwater Care Group.
- Mol, E. M., Monbaliu, E., Ven, M., Vergote, M., & Prinzie, P. (2012). The use of night orthoses in cerebral palsy treatment: Sleep disturbance in children and parental burden or not? Research in Developmental Disabilities, 33, 341–349.









